Minnesota’s Native Communities Deserve Investments in Prenatal Care

This post is the third in a new Gender, Race & Place in Minnesota series published by the Gender Policy Report that provides deeper context for the findings of the 2020 Status of Women and Girls in Minnesota report, a research collaboration between the Women’s Foundation of Minnesota and the Center on Women, Gender, and Public Policy. The data show significant health disparities affecting Native American women and girls, including higher rates of cancer, suicide attempts, and mortality from heart disease and stroke. Here, University of Minnesota public health PhD student Julia Interrante explores how systemic racism manifests in sobering disparities in prenatal care and maternal health outcomes for Native communities in Minnesota.
Walking in for my first prenatal appointment, I was full of excitement and anxiety. I had received a positive pregnancy test a few weeks before and had been anxiously awaiting the 10-week mark to have my initial prenatal visit with my doctor, the first of many visits to ensure that my baby and I were continuing safely throughout the pregnancy.
Early, regular prenatal care is essential for a healthy birth. It increases chances to prevent complications from arising and provides an opportunity to control existing health conditions, including high blood pressure and diabetes. These opportunities for prevention are especially important given growing maternal morbidity and mortality in the United States, an increase that has disproportionally affected communities of color.
Nationally, Native American women are three times more likely to die from a pregnancy-related complication than white women. In Minnesota, this disparity is almost eight times more likely compared to white women. In the midst of racial disparities highlighted by the COVID-19 pandemic and the George Floyd murder, we must make long-needed improvements in care to address the crisis of maternal health in our state.
Disparities in access to and adequacy of prenatal care
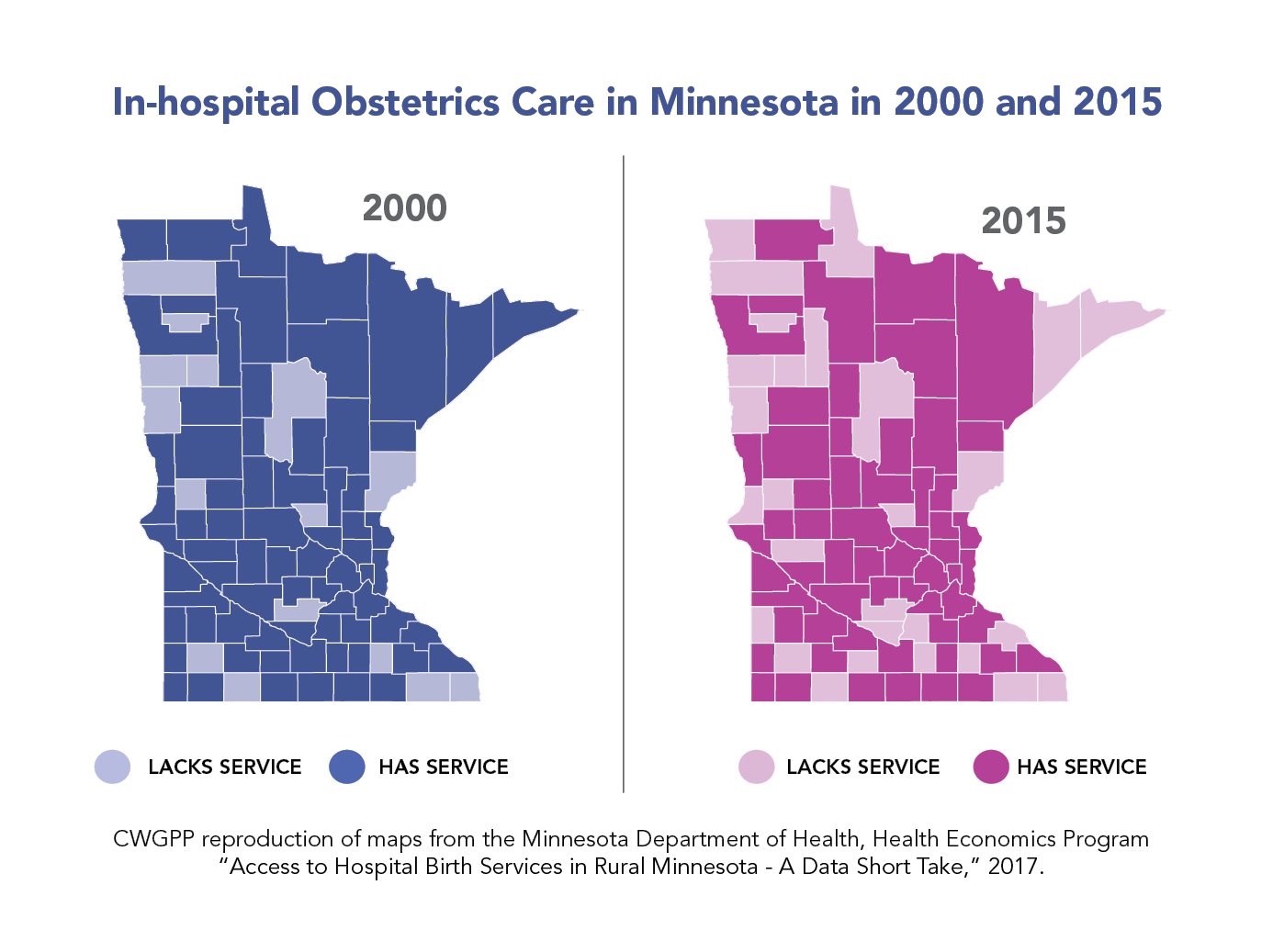
Access to prenatal care is not equal in Minnesota. While 87% of white women see a provider during their first trimester of pregnancy, as I did, this is only true for 55% of Native American women. And while early care is one side of the critical coin, having continuous care throughout pregnancy, referred to as adequate care, is the other. Disparities in adequate prenatal care are rampant: 82% of white Minnesotans report receiving adequate prenatal care, but this is only true for 47% of Native American Minnesotans. Not only is this the lowest report of prenatal care adequacy across all racial and ethnic groups in Minnesota, it represents a decrease from 2010, when 51% of Native American women reported receiving adequate prenatal care.
High rates of diabetes further complicate pregnancies
Adequate prenatal care is especially important for women who have existing health conditions like diabetes, which is the leading risk factor for poor outcomes in pregnancy, increasing the chance of mothers dying in pregnancy and increasing the risk birth defects by over 70%. Native American pregnant women in Minnesota are three times more likely to have diabetes than white women, and the rate of diabetes is growing faster for Native American women than white women.
Health counseling and planning before and during pregnancy is essential for women with diabetes to help manage the disease and ensure proper medication and monitoring. It reduces the chance of birth defects by 75%, infant death by 65%, and decreases the risk of preeclampsia for mothers by 38%. Further, interventions before and during pregnancy can decrease the risk of developing diabetes during pregnancy (gestational diabetes) by 39%.
Disparities have compounded over time

Historic marginalization and trauma of Native American communities has led to vast heath disparities, exacerbated by cumulative disadvantages in education, income, and access. Dietary changes as a result of marginalization, neglect, and relocation have led to dramatic increases in high-calorie diets and the aggregation of diabetes within Native American families.
Lack of culturally appropriate care, diabetes education and support systems, diverse and culturally competent providers, and diabetes prevention in routine medical care for Native American women all contribute to higher rates of diabetes-complicated pregnancy seen among Native American women in Minnesota.
Native Americans are more likely than any other racial or ethnic group in Minnesota to lack health insurance (23%, compared to the next highest group at 12% among Hispanic Minnesotans). Lack of health insurance and cost of care are significant barriers to diabetes screening and treatment and add to the lack of diabetes prevention and management in pregnancy.
We can do better
There are several actions that can be taken to help reduce racial disparities and improve the health of pregnant (and all) Native American Minnesotans, including increasing funding and representation.
The Indian Health Service (IHS) provides care to Native Americans living on or near reservations, but chronic underfunding means that many IHS facilities to not have the capacity to care for pregnant patients. Making money available to IHS specifically for Native American women could increase access to care prior to and during pregnancy. And while funding IHS facilities could greatly improve Native American maternal health in rural communities, 60% of Native American women live in urban areas ineligible for IHS. Only 1% of the IHS annual budget goes toward urban programs, meaning funding must be supplemented from other sources, and services are provided on a sliding-scale rather than free.
Funding should also increase for Urban Indian Health Programs like the Indian Health Board of Minneapolis (IHB). Many Native American women in Minneapolis seek care at IHB because of its culturally-centered model, established community relationships, and diverse providers. The IHB currently provides prenatal care and childbirth education and has a separate program for diabetes. It also provides transportation and Medicaid application assistance. Additional focused funding would allow the IHB to expand and focus its prenatal and preconception care programs toward diabetes prevention and treatment in pregnancy.
And ultimately, representation matters. Much of the health care workforce is not demographically reflective of the patients they treat, and Native American people are especially underrepresented. One-in-four Native American persons report racial discrimination in health care and 15% avoid care for fear of discrimination. Representation in decision-making bodies; training of health care providers on Native American history and culture, responsiveness to patient trauma, and awareness about community resources; and increasing the number of Native Americans in the health care workforce could increase access and use of pre-pregnancy and pregnancy care services among Native American communities.
As I watch my son grow, I am so grateful to the health care providers who helped ensure that I get to kiss him and tuck him into bed every night. Every pregnant person deserves this: access to the best possible care in an environment where they feel safe, supported, and understood. To have the best chance to have a healthy pregnancy, to give birth to a healthy child, and to have support for their own health and wellbeing.
While race should never be a determining factor, the truth of systemic racism is that it is. But change is possible if we invest in tangible solutions. Our Minnesota Native communities deserve it.
Julia Interrante is a graduate research assistant with the University of Minnesota Rural Health Research Center and a Health Services Research, Policy, and Administration Ph.D. student in the Division of Health Policy and Management, University of Minnesota School of Public Health. This post was originally published by the Gender Policy Report on December 15, 2020.



